Build Back Better Drug Reforms Would Lower Costs
The House-passed Build Back Better Act includes several reforms to reduce prescription drug costs for the federal government, seniors, and the public more broadly. As we’ve shown before, policymakers have a number of options available to reduce prescription drug prices.
The House bill would do so mainly by allowing the federal government to directly negotiate prices for certain drugs, limiting drug price increases to overall inflation, redesigning the Part D benefit formula, and repealing a Trump-era drug rebate rule recently delayed until 2026. Altogether, these policies would reduce deficits by $303 billion over a decade while substantially lowering health care premiums and out-of-pocket costs.
CBO’s Estimates of Prescription Drug Policies in the Build Back Better Act
| Policy | Ten-Year Savings |
|---|---|
| Medicare Drug Price Negotiations | $76 billion |
| Part B and D Inflation Rebates (Medicare and Medicaid) | $49 billion |
| Commercial Drug Inflation Rebates | $34 billion |
| Part D Benefit Formula Redesign | $2 billion* |
| Medicare Insulin and Cost Sharing Cap | -$1 billion |
| Repeal of Rebate Rule | $143 billion |
| Total Savings of Prescription Drug Proposals | $303 billion |
Sources: Congressional Budget Office and Committee for a Responsible Federal Budget.
*Includes payments for biosimilar biological products
Drug Policies in Build Back Better
The House-passed Build Back Better Act includes a number of changes to reduce prescription drug costs. Specifically, the Build Back Better Act would:
- Allow limited government negotiation of certain drugs in Parts B and D of Medicare
- Limit prescription drug price increases to the rate of inflation for drugs in Medicare Parts B and D and in the commercial insurance market
- Redesign the Medicare Part D benefit formula, including by capping annual out-of-pocket spending at $2,000 and adjusting the share of payments from insurance plans, government re-insurance, prescription drug manufacturers, and beneficiaries
- Cap the monthly copayment of insulin for Medicare beneficiaries and private insurers
- Increase rebate transparency for Pharmacy Benefit Managers (PBMs)
- Repeal the Trump Administration’s drug rebate rule that eliminates safe harbor protections for Medicare Part D rebates
Currently, the private insurance plans that provide Medicare Part D benefits negotiate prescription drug prices with manufacturers. The Build Back Better Act would allow the Secretary of Health & Human Services to directly negotiate drug prices with manufacturers on behalf of all drug plans; manufacturers who do not negotiate would face a punitive tax.
Those negotiations would be limited to small-molecule drugs that have already been on the market for at least nine years and more complex biologic drugs on the market for at least 13 years. The negotiations are also limited to just 10 total drugs in the first year (2025) rising to 20 drugs a year by 2028 and beyond, to be selected from the 50 most expensive Part B and Part D drugs. The legislation also prescribes the maximum discount allowed in the negotiation relative to current prices and depends on the number of years a drug has been on the market. The Congressional Budget Office (CBO) estimates this negotiation framework would save $76 billion over a decade, including $15 billion in 2031.
Those savings are substantially lower than in the 2019 House-passed Elijah E. Cummings Lower Drug Costs Now Act (HR 3), which saved roughly $500 billion from negotiations. That bill would allow negotiation over any brand-name drugs without generic competition among those with the highest national spending or Medicare spending. The Secretary would be allowed to negotiate 50 drugs per year with a cap on prices using an international price index and would apply Medicare-negotiated prices to the private sector. Though savings from Build Back Better would be much lower, CBO estimates a substantially smaller effect on drug innovation – with the drug pricing provisions this legislation reducing the number of new drugs by 0.8 percent rather than 4.5 percent over three decades.
In addition to allowing drug negotiations, the Build Back Better Act would also limit price increases for drugs in Medicare Parts B and D, as well as in the commercial insurance market, to the rate of inflation. This saves $83 billion – including $49 billion of savings that accrue to Medicare and Medicaid and $34 billion in higher revenue as a result of lower commercial drug prices leading to lower insurance premiums and thus higher taxable wages. Drug manufacturers would be required to send rebates to Medicare if drug prices grow faster than inflation after the benchmark year of 2021.
Build Back Better would also reform the Part D benefit formula. Specifically, it would reduce the share of drug costs covered through beneficiary cost-sharing and government re-insurance while increasing the share covered by drug manufacturers and Part D insurance plans -- particularly for "catastrophic costs". As part of this redesign, the plan would limit annual out-of-pocket costs to $2,000 per senior. The below graphic from Kaiser Family Foundation illustrates this change. Different versions of this design were proposed in President Trump's FY2020 budget, the 2019 Elijah E. Cummings Lower Drug Costs Now Act, and the 2019 bipartisan Senate Finance Prescription Drug Pricing Reduction Act. This particular redesign will save the federal government approximately $2 billion while yielding substantial savings for Medicare beneficiaries.
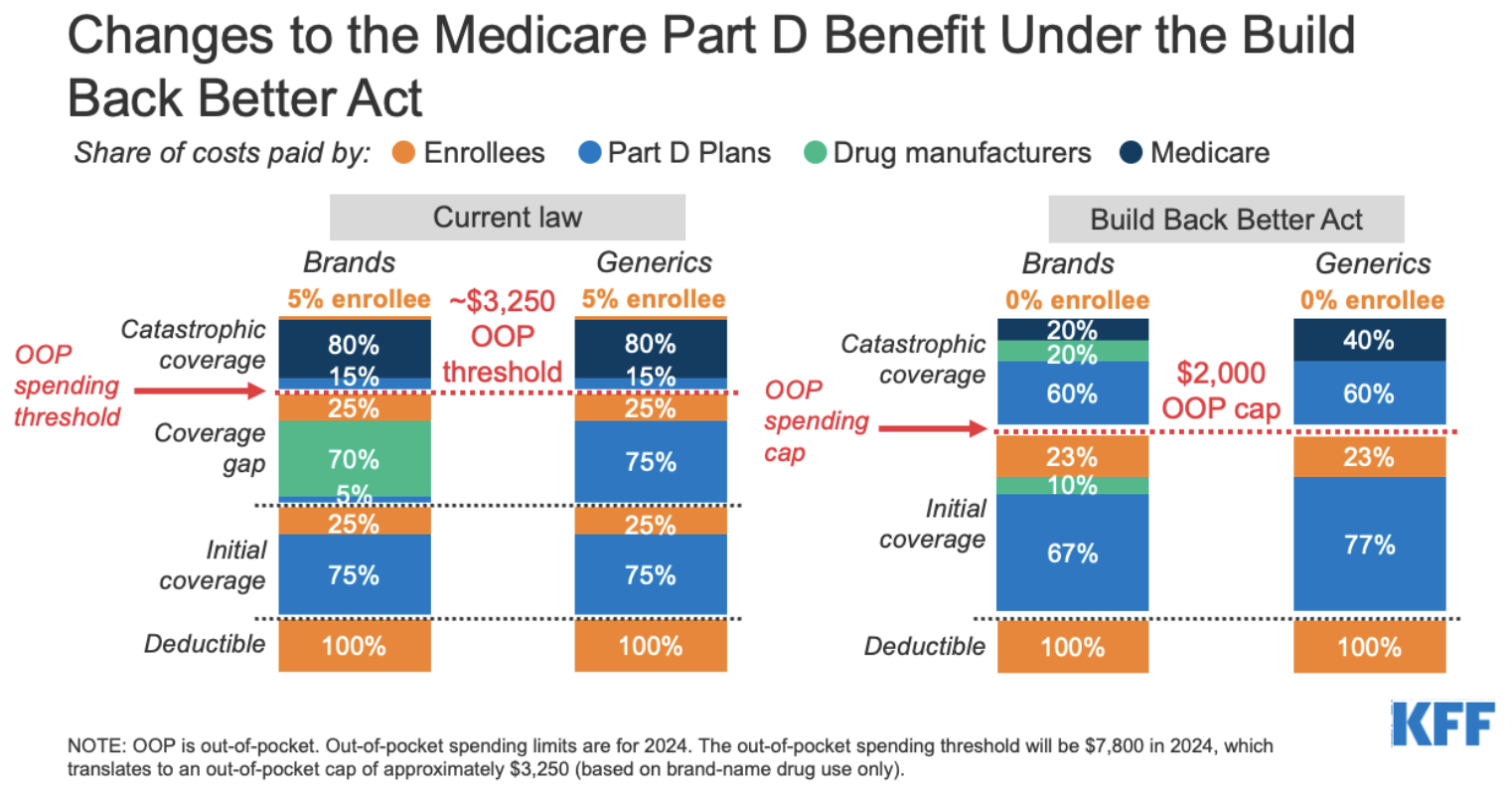
Source: Kaiser Family Foundation
The bill would also permanently repeal a Medicare Rebate Rule introduced and finalized under the Trump Administration. The rule required Pharmacy Benefit Managers (PBMs) and insurance plans to pass along drug manufacturer rebates as savings to patients, however, it was projected to increase insurance premiums and cost the federal government nearly $200 billion over a decade. This rule has been delayed until 2026 under the bipartisan infrastructure bill, saving $51 billion. The Build Back Better legislation would permanently repeal the rule and would save an additional $143 billion.
In addition, Build Back Better would cap Medicare and private insurance cost-sharing for a month's supply of insulin at $35 and require PBMs that manage drug benefits for insurers and Part D plans to disclose their rebates to employers and health plans.
Lower Drug Prices Would Generate Substantial Savings
The prescription drug provisions in the Build Back Better Act make significant reforms that lower prescription drug costs for seniors, employers, prescription drug users, and the federal government. The Congressional Budget Office estimates the proposals would save $29 billion in 2026, $61 billion by 2031, and $303 billion over a decade. This would help offset spending and tax cuts in the Build Back Better Act, including increased health care spending such as an extension of more generous Affordable Care Act subsidies, closing the Medicaid coverage gap, providing hearing benefits through Medicare, and expanding funding for home- and community-based care.
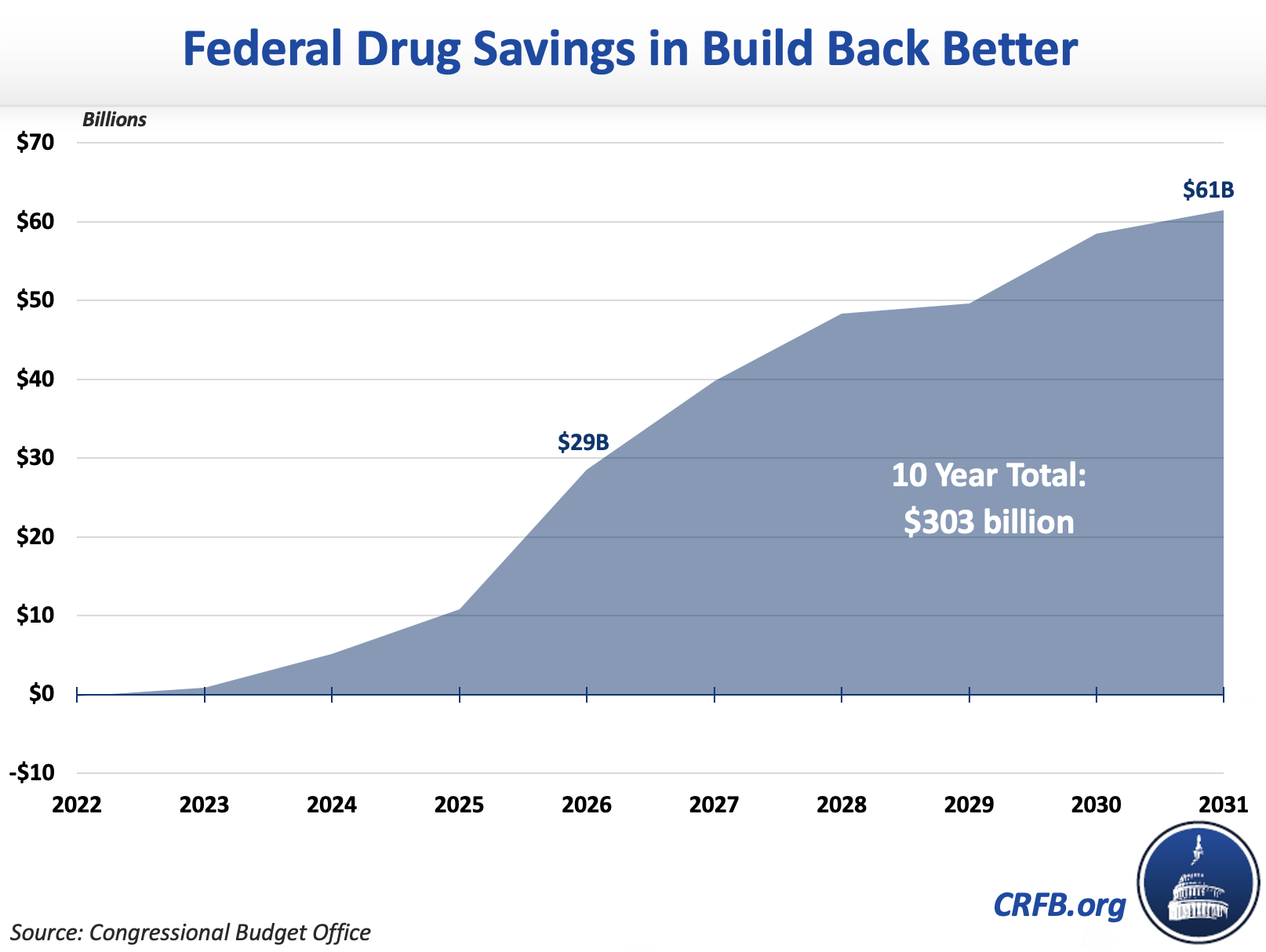
Policymakers should build on, not scale back, the savings in the House bill. More aggressive drug negotiations, inflation rebates, and benefit redesign proposals could generate tens or hundreds of billions of further savings.
There are also additional options Congress could and should consider to lower prescription drug prices, including some proposed by our Health Savers Initiative, like injecting price competition into Medicare Part B drugs and limiting evergreening for name-brand drugs. Beyond prescription drugs, numerous additional health savings related to hospitals, physicians, and Medicare Advantage plans, could reduce costs for the federal government and beneficiaries and could help to get our nation’s fiscal house in order.
With debt rising and the Medicare Hospital Insurance Trust Fund approaching insolvency, there is much work to be done to get health care costs under control. The savings in the House Build Back Better Act represent a good start.
Read more options and analyses on our Reconciliation Resources page.


