Health Spending Outlook Shows Faster Growth Ahead
The Center for Medicare and Medicaid Services (CMS) recently released new National Health Expenditure (NHE) projections through 2027, showing health spending growing slower than the economy this year but growing faster than the economy every year after that. CMS's latest projections reflect a rosier short-term outlook for NHEs but continued rapid growth in spending over the longer term.
CMS projects health spending will grow at 5.5 percent on average over the 2018-2027 period. After growing at a relatively slow rate of 3.9 percent in 2017, health spending is expected to gradually increase to 4.4 percent in 2018 and 4.8 percent in 2019 and grow in the range of 5.4-6 percent in each of the following eight years.
The 2018 and 2019 growth rates will both be below projected nominal Gross Domestic Product (GDP) growth rates of 5.2 and 4.9 percent respectively, which combined with 2017 would make three consecutive years where economic growth has outpaced health spending growth. During that period, NHEs will dip slightly as a share of GDP from 18 to 17.8 percent. However, NHE growth will be higher than economic growth every year after 2019, resulting in NHEs increasing continuously to 19.4 percent of GDP by 2027.
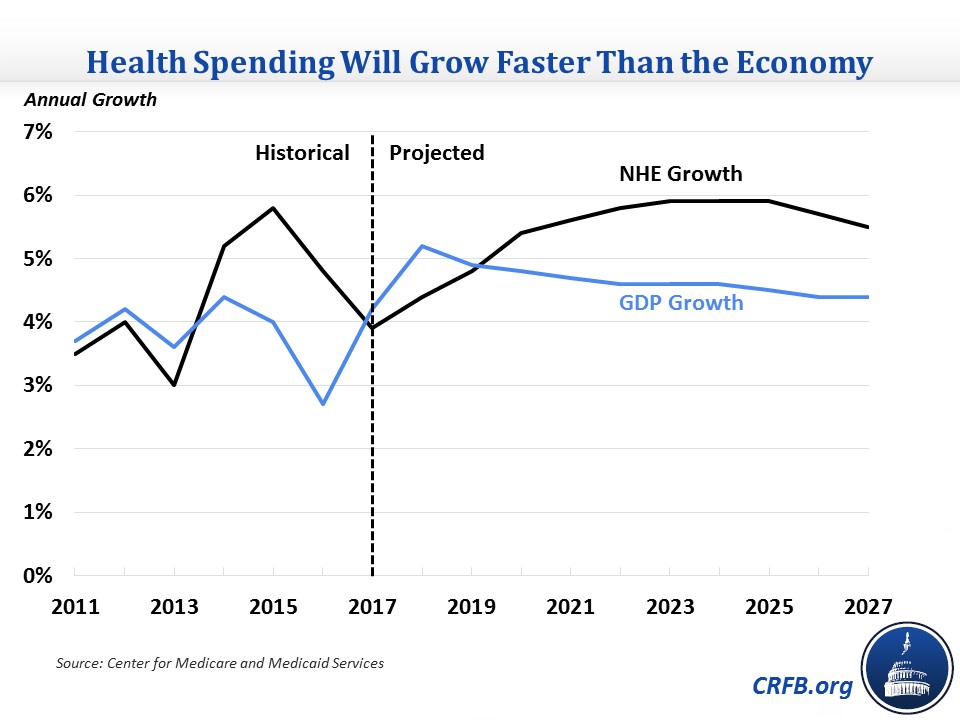
Compared to CMS's previous projection a year ago, the current projection shows lower spending both in dollars and as a percent of GDP. Total 2017-2026 spending is projected to be $421 billion (1 percent) lower in the current projection, while NHEs are projected to reach 19.2 percent of GDP in 2026 compared to 19.7 percent in last year's outlook. Most of the difference as a share of GDP comes in the near term: CMS expected NHEs to increase faster than the economy for the entire 2017-2026 period, while the current projection has NHEs growing slower than the economy for 2017-2019.

Within these overall numbers, the CMS projections provide some interesting insights related to spending growth by insurance source, the composition of NHEs, the growth in prescription drug spending, and the status of 2019 Medicaid expansions.
The Pick-Up in Spending Growth
As mentioned above, NHE growth is expected to increase from 3.9 percent in 2017 to 4.8 percent in 2019, and to remain just shy of 6 percent for the rest of the projection period. This pick-up in growth will occur across insurance sources, but to different degrees. Medicare spending growth, which has hovered between 4 and 5 percent for most of the decade, is expected to have jumped to 5.9 percent in 2018 and is projected to remain between 7 and 8 percent for the remainder of the projection period. Medicaid spending growth, which was between 2 and 3 percent in 2017 and 2018, will increase to 4.8 percent for 2019 due to Medicaid expansion taking effect in a number of states. It will stabilize at around 6 percent by 2022; CMS attributes the higher spending growth in later years to population aging. Private insurance spending, which grew between 4 and 5 percent in 2017 and 2018, will actually see its growth dip in 2019 to 3.3 percent, which CMS attributes to reduced enrollment in the health care exchanges caused by the repeal of the individual mandate from the 2010 health care law. It will hover around 5 percent after that.
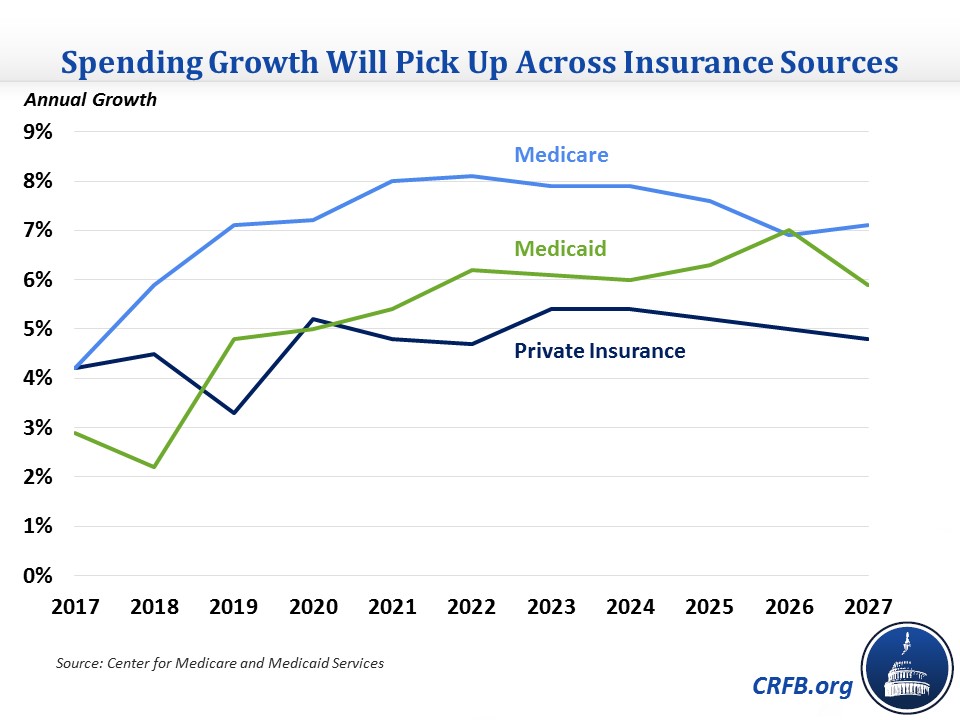
Health Spending Composition
The aging of the population is expected to drive a shift in health coverage and spending away from private insurance and towards Medicare. Per-person spending growth is projected to be relatively even across major insurance sources from 2018 through 2027, averaging 4.7 percent for Medicare, 4.2 percent for Medicaid, and 4.6 percent for private insurance. However, aging will cause the share of the population receiving private insurance to fall from 54 percent in 2017 to 50 percent by 2027, while Medicare's share will increase from 16 percent to 18 percent. Consequently, private insurance's share of NHEs will fall from 34 percent to 32 percent between 2017 and 2027, while Medicare's share will increase from 20 to 24 percent.
Prescription Drugs
Prescription drug costs have been a hot topic in recent years, and spending growth has been all over the place over the past decade. After seeing very slow spending growth in the early part of the decade, which contributed substantially to the slowdown in projected Medicare spending growth, prescription drug spending growth averaged over 10 percent in 2014-2015 due to the introduction of several high-cost specialty drugs, then dipped again to about 1 percent on average for 2016 and 2017 as the number of new products slowed. CMS expects growth to pick up again, reaching 3.3 percent in 2018, 4.6 percent in 2019, and settling in at around 6 percent by the early 2020s. It attributes the increase in growth to higher utilization related to the aging population, a greater number of new drugs being introduced, faster price growth, and more consistent treatment of patients with chronic conditions. Though NHE growth has been faster than prescription drug spending growth for much of this decade, CMS expects drug spending to grow slightly faster in the 2020s.
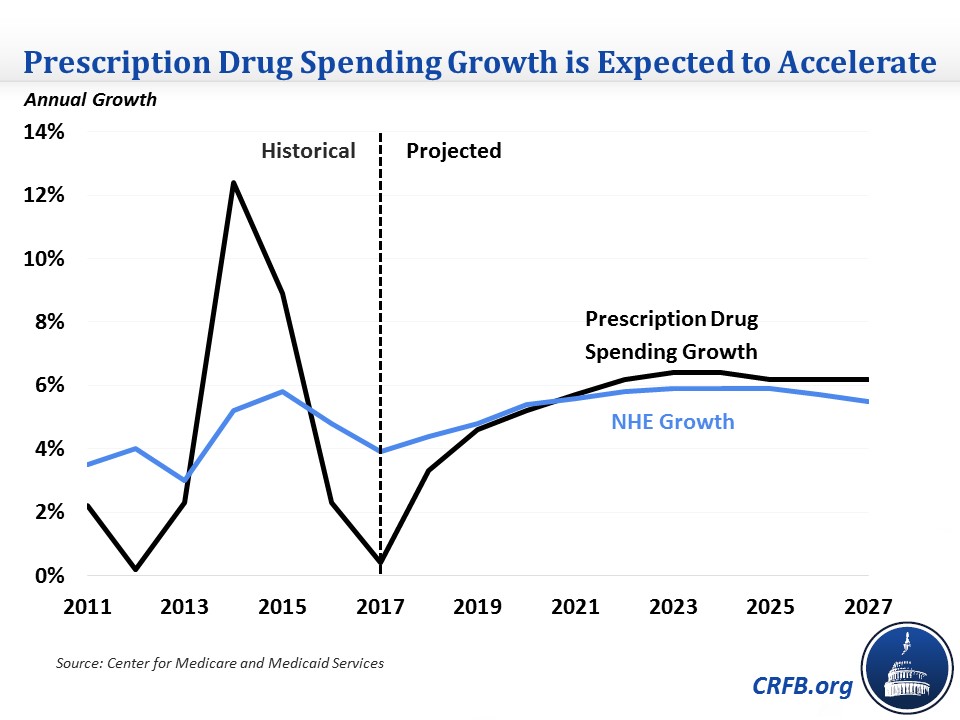
Medicaid Expansion
CMS projects that Medicaid spending growth will accelerate from 2.2 percent in 2018 to 4.8 percent in 2019, largely due to Medicaid expansion taking effect in five states: Virginia, Maine, Nebraska, Idaho, and Utah. This expansion is also expected to cause a slight acceleration in spending growth for physician services from 4.9 percent in 2018 to 5.4 percent in 2019. The Virginia legislature approved the Medicaid expansion last year and put it in into effect at the beginning of this year, while Maine's newly-inaugurated Governor Janet Mills ordered Medicaid expansion to take effect earlier this year after a 2017 ballot initiative approving it had been blocked by outgoing Governor Paul LePage. Nebraska, Idaho, and Utah all had Medicaid expansions approved by ballot initiative during the 2018 elections, but their implementation depends on what each state legislature ultimately passes. Utah has submitted to CMS a plan that would implement a partial expansion (up to the poverty line instead of 138 percent of the poverty line) with a per-person spending cap and an enrollment limit if costs exceed projections, all things that would reduce total Medicaid costs compared to a full expansion. Idaho and Nebraska's plans are less clear, but Idaho lawmakers are considering adding work requirements. Therefore, while CMS assumes full expansions will take hold this year, the reality may be more complicated and could have implications for future projections.
*****
CMS's projections show a slight decline in national health spending as a share of GDP over the past few years and in this year, but that is not expected to last. Aging of the population and other factors are expected to cause spending growth to accelerate and health spending to grow faster than the economy continuously from 2020 forward. These higher growth rates demonstrate the continued need for policymakers to explore policies that reduce health spending in public programs and system-wide.
This blog is part of the American Health Care Initiative, a joint collaboration of the Committee for a Responsible Federal Budget and the Concerned Actuaries Group dedicated to informing the public, policymakers, and key stakeholders regarding the fiscal and managerial challenges confronting our health care system. As part of the initiative, the two organizations will each publish and promote a series of papers, briefings, presentations, and other materials intended to energize a much needed conversation about improving the sustainability and accessibility of our health care system and managing the rising costs that threaten our current system.


